It’s called FESS – and these four letters mean a real relief for many a long-term sniffle. They stand for “functional endoscopic sinus surgery” and describe the most common method of controlling chronic inflammation with an operation. Anyone who thinks of deep incisions and scalpels when they hear the word “operation” can rest easy: As the name suggests, an FESS is performed endoscopically. In concrete terms, this means that a thin tube with a lighted tip is inserted through the nose for a precise and millimeter-accurate procedure from the outside. An incision through the skin is therefore usually not necessary.
When does a FESS make sense?
An operational procedure such as the FESS is usually only carried out when all other measures have already been exhausted. Depending on the cause, these include, (cortisone-containing) nasal sprays or tablets to reduce swelling of the mucous membrane but also antibiotics that are taken in tablet form to fight bacterial inflammation.
However, if nasal breathing is still restricted despite all attempts and patients suffer from constantly recurring sinus infections, then FESS can provide relief.
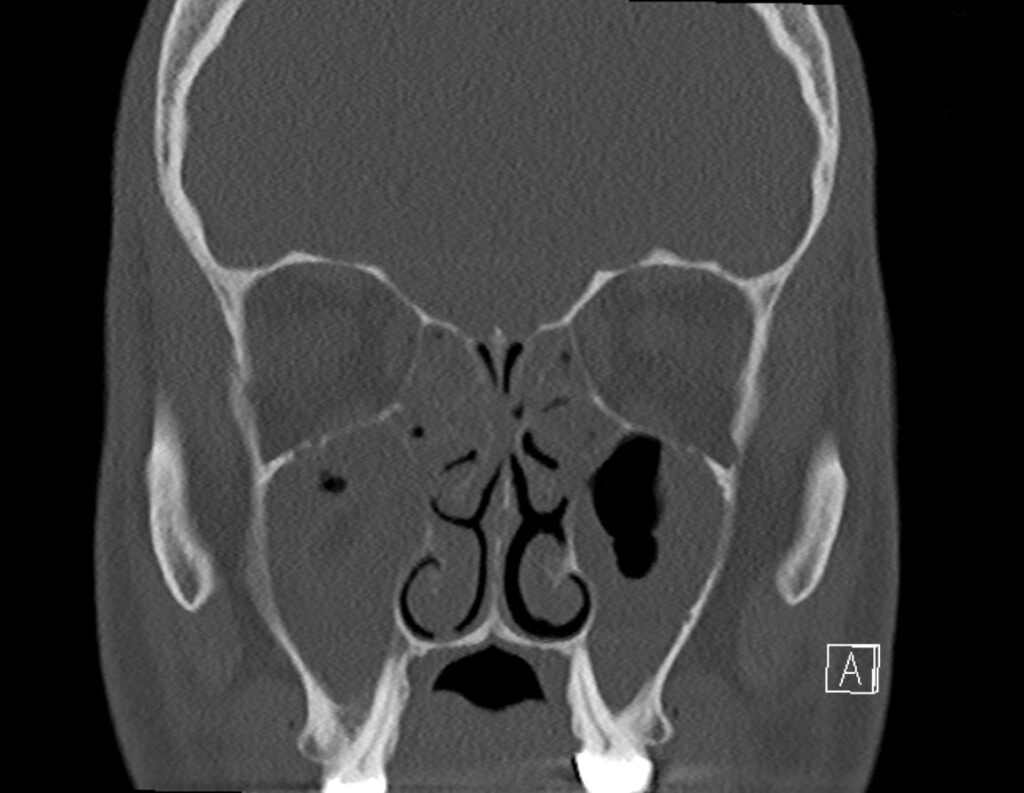
How does a FESS work exactly?
As a rule, FESS is performed on an inpatient basis in a hospital, so that patients remain on site for at least one night for observation after the procedure. Before that, there is a detailed explanation of the exact procedure and the associated risks.
The operation itself is performed under general anesthesia and usually takes between 20 minutes and two hours. There are basically three procedures to choose from, between which the surgeon chooses depending on the individual problem of the patient. The decisive factor here is which sinus is (most severely) affected:
During ethmoidectomy, infected tissue and ossification in the ethmoid sinuses are removed to create openings for ventilation. This allows the secretion to drain away unhindered – and those affected can breathe more easily. Such an artificially produced opening is also referred to as a “window”.
During an antrotomy, the entrance to the maxillary sinus is opened so that the secretion that is stuck here can flow out again and this sinus can be ventilated normally.
Shaver-supported septoplasty or turbinoplasty is about widening or straightening anatomical bottlenecks. After all, a crooked nasal septum or nasal turbinates that are too narrow can make those affected feel like they are unable to breathe properly. With the help of the shaver, tissue can be removed gently and precisely, thereby creating free space.
All three procedures aim to unclog blocked passages, flush out and loosen infectious material and thus preserve healthy tissue. As a patient, you can usually breathe more easily and regain your sense of well-being.
What are the benefits of a FESS?
For one thing, FESS is usually associated with few risks. One of the biggest advantages is that you can access it through your nose – and therefore you are spared cuts and externally visible scars. In addition, the FESS procedure is highly precise: a small camera is sent through the sinuses using a tube – while surgeons can view the inner workings in a greatly enlarged view from the outside on a screen. This enables them to work with millimeter precision, which makes FESS an overall safe and effective procedure that is performed several times a week, especially in large ENT centers.
What are the risks and disadvantages of a FESS?
Basically, a FESS is a fairly low-risk undertaking. However, as with any surgical procedure, complications can occur. In addition, general anesthesia brings risks with every operation. As a patient, however, you are informed in detail about these before you go to the operating room.
In addition, it may be necessary to repeat the procedure after a few years because the result of the FESS may not be permanent. However, in some cases, an accompanying, long-term antibody therapy can ensure that further operations are spared. The so-called monoclonal antibodies, which are usually administered by injection into the abdomen, are intended to slow down or stop inflammatory processes throughout the body. This could help those affected by stubborn inflammation that lasts for many years. Examples of active ingredients that have also proven effective in the area of the sinuses are dupilumab, mepolizumab or omalizumab. However, access to such therapy is not easy and patients must meet certain criteria to be eligible. It is best to discuss this idea with the treating ENT.
FESS should not be the first line of treatment used for sinusitis. However, if other ways have not led to the goal or at least alleviated the limitations, it can be an effective means of being able to breathe easier in the long term.
Feel free to contact me and book your appointment conveniently online now.
Sources:
● Medtronic GmbH, 2017: Nasennebenhöhlenentzündung. Retrieved via https://www.medtronic.com/de-de/patienten/produkte-therapien/nasennebenhoehlen-entzuendung.html on 04/04/2023
● Medizin kompakt, o.D.: Ehtmoidektomie. Retrieved via https://www.medizin-kompakt.de/ethmoidektomie on 04/10/2023
● Dr. Seidel, 2021: Kieferhöhlenentzündung. Retrieved via https://www.zahnarzt-drseidel.de/kieferchirurgie/kieferhoehlenentzuendung/ on 04/06/2023
● Primo Medico GmbH, o.D.: Nasennebenhöhlen-OP. Retrieved via https://www.primomedico.com/de/behandlung/nasennebenhoehlen-op/ on 04/06/2023